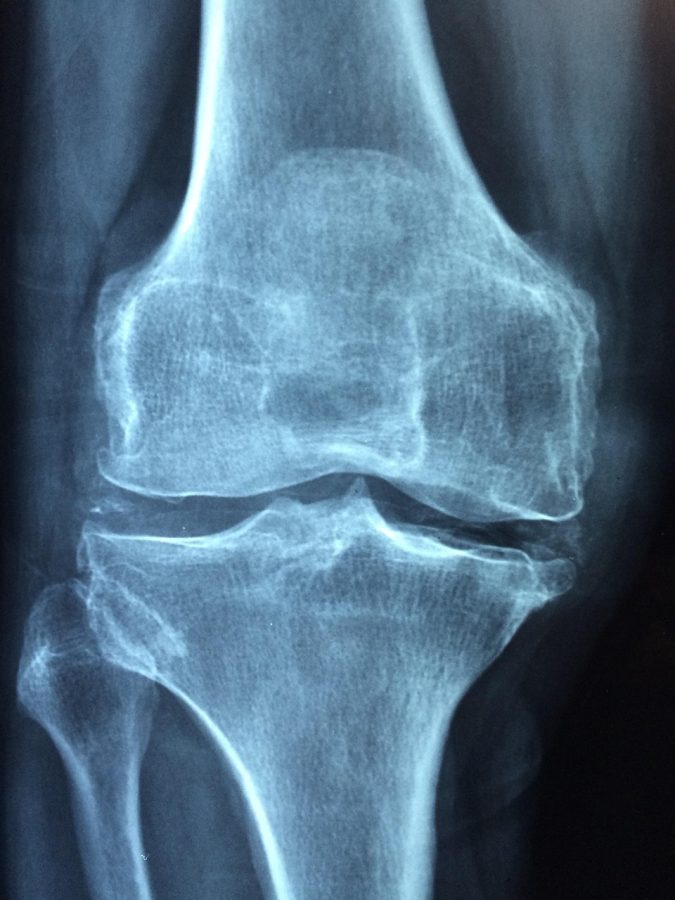
Arthritis in your 40s can begin quietly, often showing up as morning stiffness, swelling, or aching joints that linger. The earlier you notice the pattern and respond with realistic changes and proper medical care, the easier it is to slow progression and stay active.
Quick Action Plan
- Track symptoms like stiffness or swelling that last more than two weeks.
- Adopt low-impact exercise such as cycling or swimming to protect your joints.
- Consult a doctor early to confirm diagnosis and start treatment if needed.
Sources: Harvard Health, Mayo Clinic, NIH/NIAMS
Arthritis in your 40s can feel confusing because it often starts without a clear “event.” It’s not always sharp pain. Sometimes it’s just stiffness that lasts a little longer than it used to, or a joint that needs more time to warm up. The hard part is figuring out what’s normal fatigue and what’s a pattern that deserves attention.
Why does arthritis start in your 40s?
Because the body’s recovery margin gets smaller, and cartilage plus old injuries react more strongly to everyday load.
By your 40s, your joints often feel the cumulative effect of years of work, training, sitting, driving, and small injuries you once forgot about. Cartilage naturally thins with age, muscles may protect joints less unless you maintain strength, and extra body weight increases pressure. Arthritis in your 40s is rarely caused by one single thing. It’s usually years of normal habits meeting a body that now plays by slightly different rules.
That’s why early signals matter. Not because you need to panic, but because making adjustments early is often easier than trying to fix everything later when movement already feels unreliable.
What are the early signs of arthritis in your 40s?
Morning stiffness, swelling, tenderness, and pain that lingers after rest are common early signs.
Early arthritis doesn’t always look dramatic. Many people describe it as stiffness that “hangs around” instead of fading quickly, or a dull ache after activity that takes longer to calm down. Joints may feel tight after sitting, and sometimes there’s mild swelling you only notice when you compare sides. If this repeats week after week, it’s more likely arthritis in your 40s than a one-off bad day.
People often confuse these signs with simple fatigue. But if stiffness regularly lasts more than about 30 minutes in the morning, or symptoms keep returning after normal daily activity, it’s worth taking seriously rather than just pushing through it.
How does arthritis in your 40s affect daily life?
It can quietly limit mobility, make stairs harder, and add fatigue and hesitation to simple tasks.
For many adults, arthritis in your 40s doesn’t “stop” them. It slows them down. Stairs start requiring more attention. Getting up from a chair takes a second longer. Long walks feel less predictable. You still do everything, but you’re more aware of your joints while doing it.
Over time, this can turn into cautious movement. People begin avoiding certain motions without fully realizing it, and that often leads to more stiffness and weaker supporting muscles. The earlier you interrupt this cycle, the easier it is to stay active and independent.
What types of arthritis can begin in your 40s?
Osteoarthritis, rheumatoid arthritis, and gout may all start in your 40s.
Not all arthritis is the same, and this matters more than people expect. Osteoarthritis is the most common and is strongly connected to mechanical wear and load over time. Autoimmune conditions like rheumatoid arthritis can also begin in this decade and often come with swelling, prolonged stiffness, and symptoms that may affect both sides of the body. Gout can appear as sudden, intense flares that feel out of proportion to recent activity.
Because symptoms overlap, arthritis in your 40s is not something to self-diagnose by guesswork. The type influences what treatment is appropriate and what might actually make things worse.
Is arthritis in your 40s genetic or lifestyle-driven?
It’s usually a mix of both: genetics can raise risk, and lifestyle often determines how fast symptoms appear.
Family history can set the stage. But lifestyle often decides how quickly joints become symptomatic. Body weight, muscle strength, activity level, and the way you move every day can either protect joints or overload them. Many people don’t realize how much “normal life” load adds up until arthritis in your 40s makes it visible.
The helpful mindset is practical: you can’t change genetics, but you can often change the direction of the next few years with small, consistent adjustments.
How is arthritis in your 40s diagnosed?
Through a clinical exam, imaging (often X-rays), and sometimes blood tests, ultrasound, or MRI.
Diagnosis usually starts with a clinical exam, your symptom history, and a look at how the joint behaves in movement. X-rays can show joint space narrowing and other changes, while blood tests can help identify inflammatory forms. Ultrasound or MRI may be used in specific cases, especially if symptoms are unclear. If joint pain keeps returning and function is changing, getting clarity early tends to make the rest of the process simpler.
Can exercise reduce arthritis pain in your 40s?
Yes—smart, low-impact movement and strength work can reduce stiffness and protect joints.
This is one of the few areas where the answer is genuinely encouraging. Regular movement helps joints stay mobile, and strength training improves stability so the joint is not taking all the load alone. Low-impact options like walking, cycling, and swimming are often easier on irritated joints, especially at the beginning. The key is not heroic workouts. It’s consistency and a plan that your body can recover from.
For many people with arthritis in your 40s, exercise doesn’t remove every sensation, but it often makes daily life feel more predictable again.
What role does diet play in arthritis in your 40s?
Diet can influence inflammation and body weight, both of which affect joint pain and flares.
Diet won’t “cure” arthritis, but it can meaningfully affect symptoms. Keeping weight in a healthier range reduces joint load, and certain eating patterns can support lower inflammation. Many people do better when they prioritize vegetables, fiber, omega-3-rich foods (like fatty fish), nuts, and olive oil, and reduce ultra-processed foods and sugary drinks.
The most useful approach is simple: eat in a way that supports stable energy, healthy weight, and steady recovery. It’s not about perfect rules. It’s about giving your joints fewer reasons to flare.
When should you see a doctor for arthritis in your 40s?
If pain lasts more than two weeks, limits mobility, or is paired with swelling, warmth, or fever.
Two weeks isn’t a magic number, but it’s a useful line in real life. If symptoms persist, keep returning, or start limiting movement, getting evaluated early can prevent long-term damage. Swelling, warmth, visible inflammation, or systemic symptoms like fever should be taken more seriously and checked sooner rather than later.
Arthritis in your 40s is not something to ignore until it becomes severe. Early clarity often saves time, money, and stress.
What treatments help arthritis in your 40s?
Exercise, physical therapy, medication when needed, and lifestyle changes are common first-line treatments.
Most treatment plans start with practical foundations: movement, strengthening, mobility work, and weight management. Physical therapy can help you rebuild joint-friendly movement patterns. Doctors may also recommend pain relief options such as NSAIDs, and in some cases injections or disease-specific medications depending on the type of arthritis.
What tends to work best is not a single tool, but a long-term plan you can actually follow. The goal is to keep arthritis in your 40s from narrowing your life little by little.
Related Articles
- Joint Pain After 40
- Hip Joint Pain at 40
- Why Do Joints Crack?
- Why Do Legs Hurt After 40?
- Why Do My Legs Hurt So Bad?
FAQ: Arthritis in Your 40s
Is arthritis in your 40s common?
Yes, many adults start to notice early arthritis in their 40s, especially if risk factors exist.
Does weight loss help arthritis in your 40s?
Yes, losing 5–10% body weight reduces pressure on joints and lowers pain.
What vitamins support joint health?
Vitamin D and omega-3s may help if deficient, but food first is always best.
Take Care of Your Joints Today
Your 40s are a good decade to act, not because you’re “old,” but because small patterns become louder over time. Notice what repeats, keep your joints moving in joint-friendly ways, build strength gradually, and get medical help when symptoms persist. Done early, these steps can protect your mobility and keep arthritis in your 40s from quietly limiting your life later.